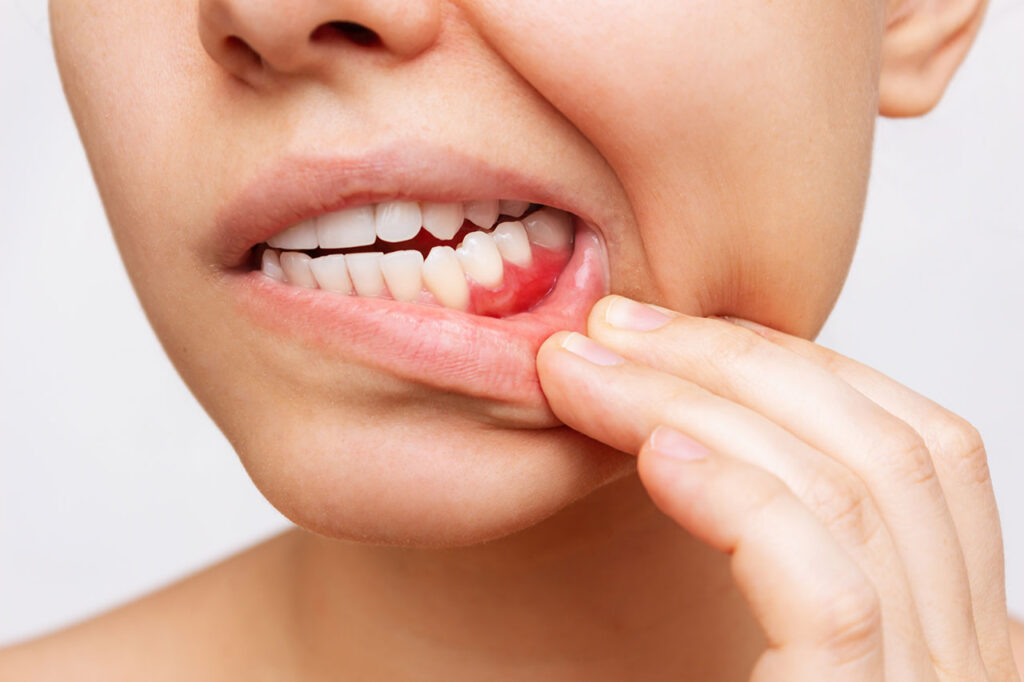
If your gums bleed when you brush or floss, it’s tempting to shrug it off. “I must’ve brushed too hard,” right? Sometimes, sure. But frequent bleeding is often your gums waving a little red flag: inflammation is present, and periodontal disease may be starting. The tricky part is that gum disease can progress quietly—while your teeth still look fine—until bone support is affected.
This guide walks through what periodontal disease is, the early warning signs, what treatments like scaling and root planing actually do, and how to keep your gums healthier for the long haul.
What Periodontal Disease Really Is (And Why It Matters)
Periodontal disease is an infection and inflammatory condition that affects the gums and the bone that supports your teeth. It usually begins as gingivitis—gum inflammation caused by plaque build-up at the gumline. Gingivitis is common and often reversible with improved hygiene and professional cleanings.
If plaque sits long enough, it hardens into tartar (calculus). Tartar makes it easier for bacteria to cling to teeth and slip under the gums. That’s when gingivitis can progress to periodontitis. In periodontitis, the gums pull away from the teeth, creating “pockets” where bacteria thrive. Over time, the body’s inflammatory response and bacterial toxins can break down bone. That bone loss is what leads to loose teeth and, in advanced cases, tooth loss.
Periodontal disease also has a “whole-body” angle. Chronic inflammation in the mouth has been associated in research with systemic health concerns, including diabetes control and cardiovascular risk. It’s not that gum therapy “cures” other conditions, but controlling oral inflammation supports overall wellness.
Early Warning Signs People Miss
Gum disease isn’t always painful at first, which is why it’s so easy to ignore. Common signs include:
- Bleeding when brushing or flossing
- Swollen, puffy, or tender gums
- Gum recession (teeth looking longer)
- Persistent bad breath or bad taste
- Sensitivity near the gumline
- Changes in bite or spaces between teeth
- Loose teeth (later stage)
A helpful mindset: healthy gums usually don’t bleed with gentle daily flossing. If bleeding happens consistently for more than a week or two, it’s worth a check.
Why Brushing Harder Can Backfire
When gums bleed, many people either stop flossing (so the area stays inflamed) or brush harder (which can irritate tissues and contribute to recession). The better approach is gentle consistency: soft bristles, small circles at the gumline, and daily cleaning between teeth. If the bleeding is from gingivitis, it often improves after a week or two of steady care plus a professional cleaning. If it doesn’t improve, that’s where deeper evaluation comes in.
The “Deep Cleaning” Explained: Scaling and Root Planing
Scaling and root planing is a periodontal therapy often recommended when pockets have formed and bacteria and tartar are present under the gumline. People call it a “deep cleaning,” but the name can make it sound scarier than it is.
- Scaling removes plaque and tartar from above and below the gumline, including inside gum pockets.
- Root planing smooths the root surfaces so gums can reattach more closely and bacteria have a harder time sticking.
Local anesthetic is typically used to keep you comfortable. The mouth may be treated in sections, depending on how much area needs attention. Afterward, the gums may feel tender for a few days, and you may notice less bleeding and less puffiness as inflammation calms down.
Scaling and root planing is not cosmetic. It’s infection control. It aims to reduce pocket depth, lower bacterial load, and stabilize the foundation that holds teeth in place.
What Happens After Treatment (The Part That Decides Success)
Periodontal disease is a “management” condition. That isn’t bad news—it just means follow-up matters. After scaling and root planing, your dentist will re-check pocket depths and gum health. Many patients transition to more frequent periodontal maintenance cleanings (often every 3–4 months) for a while, because bacteria can repopulate pockets faster than in a healthy mouth.
Home care becomes non-negotiable:
- Brush twice a day with fluoride toothpaste
- Clean between teeth daily (floss, interdental brushes, or a water flosser)
- Consider an electric toothbrush for more consistent plaque removal
- If recommended, use an antimicrobial rinse short-term (not forever, unless instructed)
Lifestyle factors matter too. Smoking and vaping increase periodontal risk and slow healing. Managing blood sugar helps gums heal better. Dry mouth can increase bacterial growth. These aren’t “moral” issues; they’re biology.
Benefits, Supported by Professional Sources
Professional organizations like the American Dental Association (ADA) and the CDC highlight that gum disease is common but treatable—and that early care prevents progression. The National Institute of Dental and Craniofacial Research (NIDCR) notes that periodontitis can damage the bone that supports teeth, which is why evaluation and treatment are important.
Peer-reviewed research supports scaling and root planing as an effective first-line therapy for reducing inflammation and pocket depth in many cases of periodontitis. Studies consistently show that improved plaque control plus professional periodontal therapy can stabilize disease and reduce bleeding and swelling. The earlier treatment begins, the more predictable the results typically are.
Prevention That Fits Real Life
Let’s keep it practical. If you want healthier gums, focus on the few actions that move the needle:
- Brush the gumline, not just the teeth. Aim bristles where tooth meets gum.
- Clean between teeth once daily. Not “when you remember.” Daily.
- Make water your default drink. Frequent sugary sips feed bacteria all day.
- Stay consistent with checkups and cleanings. Gum disease thrives on long gaps.
- Ask about tools. Interdental brushes can be easier than string floss for some.
- Wear a night guard if you clench. Clenching doesn’t cause periodontal disease, but it can worsen mobility in already weakened support.
Common Questions People Ask About Periodontal Disease
Can gums grow back? Gum tissue doesn’t “regrow” like hair. But inflammation can shrink back down, and healthy gum attachment can improve after therapy. In cases of significant recession, gum grafting may be considered.
Is scaling and root planing the same as a regular cleaning? No. Routine cleanings focus on above-gum buildup. Scaling and root planing treats below-gum infection and pockets.
Will I need antibiotics? Sometimes, but not always. Your dentist decides based on infection severity, pocket depth, and overall health.
Does gum disease always lead to tooth loss? Not if it’s managed. Many patients keep their teeth for life with the right care plan.
A Better Way to Think About It
Gum health is like a foundation. You don’t see it every day, but it holds everything up. If the foundation is strong, crowns, fillings, implants—everything—last longer. If the foundation is inflamed, even great dentistry has a harder time.
If you’re noticing bleeding, bad breath that doesn’t improve, or gums that look puffy, it’s worth getting answers. Schedule a Consultation with All About Smiles in Rogers, AR, or call 870-669-1507 to Book an Appointment.